


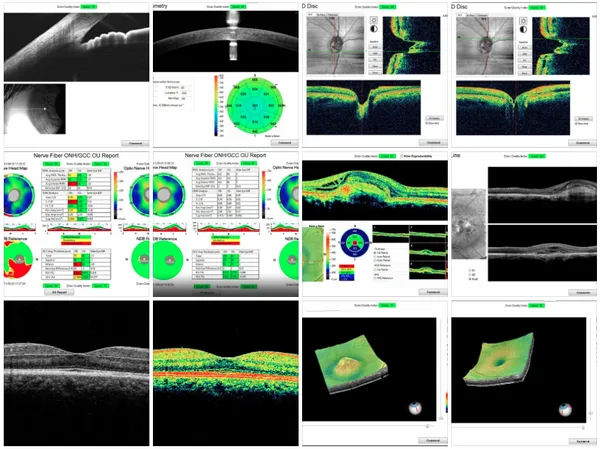
Onsite~ In our Refractive/ Ocular treatment suite
The P.A.M. or Potential Acuity Meter (Retinometer) - this instrument is used to assess potential visual acuity in persons with cataracts and other opacities. In other words remove the cataract and anticipate this corrected vision level limited by say Macular Degeneration or Amblyopia. The available acuity scale runs 20/25 to 20/300.This is assuming any corneal media opacities are by passed.
The Pachymeter – this measures corneal thickness utilizing Ultrasound; this has relevance to prospective Lasik patients, Glaucoma screening and management, cataract patients and other corneal thinning diseases (ectatic diseases) – ie; Keratoconus.
Digital Sphygmomanometer – this provides info about pulse, Systolic and Diastolic B.P. relevant to assess current Pulse pressure levels and their potential deleterious effect certainly on Macular Degenerative patients but also, Diabetic, confirmed and yet to be confirmed Glaucoma patients going forward. B.P. testing has relevance to patients with Normal Tension Glaucoma. It is also a nice addition to the Primary Eyecare Generalists ability to assist in the management of mutual Diabetic patients. B.P. testing may for the first time reveal HTN in a person who does not seek proper healthcare and is manifesting signs of an impending stroke.* Recently The College for B.C. Optometrists has mandated that all Patients Initially Diagnosed with Glaucoma must Initially and on going have their B.P. monitored as well as having their eyes drainage angles assessed and their Corneal Thickness Determined: all this before initiation of treatment. **Corneal thickness measurement is called Pachymetry and more correctly stages the starting Intra Ocular Pressure level in each of a patients eyes. This from the** O.A.T.S study.Pt B.P is relevant to choice of Treatment Medication as is Pt’s Respiratory and Cardiovascular Status. A new Glaucoma combo drug has come online that does not involve Timoptic or any beta blocker but rather Alphagan and Azopt as a fixed dose suspension offering a 30% reduction in IOP. So it will indeed prove helpful here when heart rate and respiration is a factor.
THE Pascal Tonometer – This machine is explained under the discussion for Glaucoma.
Onsite – In our Ocular Imaging Suite
Digital Retinal Imaging – This is probably the greatest tool available to the Optometric today, rivalled only by the High Def O.C.T. This technology has evolved to permit a 50-degree view of the retina often without use of dilating drops. Very small Drusen or non-functioning RPE Cell castoff debris can be seen and documented that do Macularly correlate beautifully with the PHP tests resultant distortion localization. Very small micro aneurisms in Diabetic Retinopathy can be revealed. Tons of retinal anomalies can be revealed and documented for possible progression or sent out for immediate treatment. The Optic Nerve head can be reviewed for visible changes suggestive of Glaucoma. and/or other neuropathies. Vascular changes can make inferences about B.P and cholesterol management.
The H.D. OCT. – NOW ONSITE after 6 years of research and planning: the once missing and greatly essential equipment piece to unlocking and gaining an understanding of the earliest detection and management of several Retinal Diseases .The High Definition O.C.T. aka Spectral Domain O.C.T. has indeed launch Retinal Eye Disease detection, monitoring and management into another galaxy. In literally seconds you can acquire packets of information cubes that reveal subtle details of pathology at specific retinal levels with clear concise reproducible documentation. The machines can scan to a retinal depth of 5milli microns, at a rate of 26,000 A scans per second. The high speed laser enables maintenance of patient focus such that summated reflections of the over passing laser light A scans build packets called B scans that when added together yield cubes. From these retinal thickness maps can be constructed for any retinal level be it from the ILM (Internal Limiting Membrane) to the R.P.E.(The Retinal Pigmented Epithelium). You can be very specific and quantify edema and or depositing at each macular level. You can Pinpoint Macular Drusen as to quantity. You can analyse the effect an epi retinal membrane is having on Macular integrity as to whether surgery may be required. Macular edema can accurately be assessed in Hard to control Diabetics. High Definition cross sectional cuts of the Optic Nerve head are used to screen, monitor and manage Glaucoma Patients. In the years to follow the High Def will replace the Gold Standard bearer H.R.T. in Glaucoma management as it will reveal the earliest Glaucoma changes at the macular level and will be fitted to analyse blood flow dynamics associated with the Retinal diseases of Glaucoma, Macular degeneration and Diabetes to name a few. Indeed very exciting stuff going forward. The detailed insights provided by the High Def O.C.T are so illuminating that it’s been regarded by many as an M.R.I of the Eye. This laser will not damage one’s eyes.
Onsite- In our Ocular Perimetry Suite
The P.H.P. It is called The Foresee P.H.P. ( PHP means Preferential Hyperacuity Perimetery ) What hyperacuity or ( Vernier acuity ) really speaks to is the ability to detect a minute difference in the spatial location of 2 or more stimuli. Here in a pre -determined area of 14 by 14 degrees we project a dot deviated signal expecting a specific response in the retinal receptive fields. If the stimuli encounter a Drusen (an area of devitalized cells) which in turn elevates the retinal pigment cells upward at that location instead of receptor field 5,6 and 7 firing: 5,6 and 9 record. You get a resultant bowing of the photoreceptor layer and The image to the patient will appear distorted or (metamorphic). With this brilliant non- invasive 5 minute test we can detect AMD, monitor its progression to include early detection of its conversion to choroidal neovascular or wet AMD where the protective bloodbrain barrier is breached by choroidal vessels from below that now leak into the RPE space. If left untreated scaring and massive vision loss ensues. The PHP is therefore a sequential test over the year looking for change, versus stability. When discovered wet AMD is treated usually with 1month to 7 week multiple AVASTIN and some times LUCENTIS injections to preserve and slightly improve current measurable Pt. vision levels over about a 2.5 to 4 year course of treatment.
THE VISUAL FIELD ANALYZER (Humphrey et al) – here central and peripheral fields of vision are assessed. This has relevant application in Glaucoma screening and management. Testing can reveal the presence of masses that impinge on the visual system apparatus ( ie: Orbital Tumor ); can document the effects of a stroke on visual field and reveal the effects of Multiple Sclerosis on the Optic Nerve as well as to reveal the effects of several retinal disorders on visual field. It also can be used to determine visual competency to drive and can illicit the effects of certain high risk meds on visual function. Such as Plaquinal use for Arthritis and Gabapentin ( Neurotin ) and others.
OFF SIGHT EQUIPMENT : AVD
(THE H.R.T.) or The Heidleberg Retinal Tomograph – This current Gold standard in Glaucoma determination and progression management is quickly losing ground to the future of the High Definition O.C.T. This is a con-focal laser system that reveals 3D images about the posterior segment. This in turn is the value asset at the back of the eye. This machine will pick up the earliest Glaucoma damage. There will be a loss of nerve fibers such that the 3D scanned image of the Optic Nerve Head will reveal sequential changes among successive scans. The nerve fiber loss in turn will go onto reveal an eventual loss of visual field. What is found regarding Nerve Head changes by the HRT may precede actual field of vision testing changes by 6 to 8 years. When persons are deemed to fit in the at risk group for Glaucoma, HRT’s are usually initially 3 to 6 month intervals until a basis is established. There are about 6 important parameters that are looked at for change over time to signify ( Progression ). My own personal findings are that the current OCT technology can allow one to formulate a decision about patient Glaucoma applicability 3 to 4 years ahead of the HRT having sent numerous patients out for such tests over that time frame with no reveal and then to diagnose them on the first OCT scanning session. Needless to say we have for all patients replaced HRT out sourced visitations by our in house OCT.
THE A SCAN – This employs ultrasound Biometry ( The length of the Eye is measured using emitted sound ). This is done so that the correct intra ocular lens to achieve the final correct Rx is determined .It works on the assumption that the Eyes entire power is 60 Diopters which the Cornea contributes 40 diopters and the lens the other 20 diopters. Using the corneal interpretation and the axial A scanned length in a formula the Final IOL or intra ocular lens power is available to the Surgeon. The A scan also proves helpful in understanding why some Myopes OCT results are worse than expected do the magnification effect of the optic disc that can confuse the OCT in deriving boundaries for the Optic nerve head. Similarly a high Hyperopes short eye will evoke a false minification and OCT results will appear better than they are in fact. Rule of thumb when in doubt assume very long and short eyes cause imaging inaccuracies. Resultant A scanned lengths will support or refute your hypothesis here.
THE PENTACAM - ‘The Gold Standard’ in Corneal Topography. In a record 2 seconds it generates a corneal map from 25,000 corneal elevation points. It has the ability to interpret both the anterior and posterior corneal surfaces. The latter is important in Pre Lasik evaluation. This can reveal a patient at either early or late stage Keratoconus ( a corneal thinning disease ), It can also read thickness at different specific loci. Lastly and very important the Pentacam generated info has relevance to post Lasik patients that now require cataract surgery specific to intra ocular lens calculations. Lastly it also can predict future problems in maintaining Corneal clarity in post cataract patients. Again I have to elucidate that the with some and not all newer OCT’s an anterior lens can be affixed to give some this same information and also speak to the configuration of the anterior drainage angle.* The very latest addition was an added on retinal camera. Good if you do not yet have one. Still to come in the future is the OCT with the Sapphire Blue laser that will scan to 2milli microns of tissue depth yielding images that will be shocking clear in detail and the development of non -dye injected O.C.T. Angiography that will record blood flow at the Optic Nerve Head and will be helpful in staging and altering successfully the course of Glaucoma progression over all Glaucoma types. Since I wrote this it was revealed to me that Optovue U.S.A. has developed an O.C.T. that records blood flow and thus records Ocular Nerve Head perfusion. They found that A Glaucomatous Eye has a 19% reduction in Blood Flow and that reduced blood flow correlates with declining visual field as indicated by the indices the P.S.D. on visual field testing printouts. ( David Huang Ophthalmology Times 2013 ). This Experimental O.C.T.’s can also scan to 5 milli-micron depth at a speed of 100,000 A scans per second using SSADA technology (swept-source O.C.T.). Unbelievable! {Revealed at Vision West 2013}. Optovue has a commercial version that scans at 70,000 scans per second that will be fast enough to run this future application called the Avanti Wide Field. The take away is that this is leading to an understanding that vascular insufficiency precedes Glaucoma damage. The Wide field will measure blood flow at the Short Posterior Ciliary arteries. Doppler OCT can only speak to general flow and true Fluorescein with dye contrast deals with much larger vessels than either of these two. Some Canada available Combined Glaucoma Meds contain a Beta blocker that should not be given after dinner owing to nocturnal hypotension as a possibility. In the same way Beta Blockers have been moved away from in Blood pressure management for a large part especially if Glaucoma is aPossibility or is Sleep Apnea exists.
THE YAG LASER (Yag Laser Capsulotomy) – information sources state that 30% of Post patients develop a (PCO), a posterior capsular opacity. I think from my experience this number is more realistically 80%; possible explanation the surgeon does not follow the patient far enough out over time .Here what happens is that Epithelial cells have grown or migrated over the posterior lens capsule to evoke a hazy membrane. (a sort of after the surgery then again cataract effect). In deciding to yag a patient the surgeon is aware that Retinal Detachments occur at 1%* of cataract surgeries and 2 % of patient Yags. For about 2 weeks after the Yag the patient reports an awareness of floaters.* This RD risk is higher if the patient is Myopic and under 60 years; approximately 2%.Rule of thumb younger myopic cataract patients require closer post cataract surgery retinal scrutiny for possible tears or detachment.
The S.L.T. (Selective Laser Trabeculoplasty) – This has been well received by the Eye Surgeon community. Some even offer it as a first line rather than an intermediate in Glaucoma management. The past GLC protocol was Meds then SLT/ then Filtration Surgical Procedures .For the person who is intolerant to the irritation of Travatan Z and has become Non compliant to care directives or when cost of Meds are a big factor SLT helps. The way to get around the irritation of Travatan Z is the newest arrival of a preservative- free Prostaglandin Analog called Zioptan. Not available in Canada yet. Possibly do to costly unit vials system requiring refrigeration. Just because someone has had S.L.T. and is off Meds for the moment does not mean that they will never return to Meds as required adjunct therapy. So possibly they will need them after SLT is exhausted. With SLT what happens is that a Low pulse Laser light is directed on the Melanin cells in the channels; the channels being the Trabecular Meshwork. Fluid outflow is enhanced but this may not last over time such that the patient is returned for a retreatment full or partial with a IOP reduction less favorable than the first application if it fact works for said patient at all the second time. Most probably the patient returns to drops in 5 years or they go onto an anterior chamber valve. Unfortunately the co-managing practitioner will find SLT patients think they are one time fixed and therefore do not need on going Glaucoma management. Not the case they should keep up their office visitations as requested of them. This is where the platform of decided tests over a year helps with patient compliance. Drugs will probably again retake front and center first line choice even by those advocating laser Glaucoma treatment by means of SLT as first line when all treating communities have access to a New classification of Glaucoma meds called Rho Kinase Inhibitors (ROCK) that actually act right at the trabecular mesh works canals increasing outflow by reducing its canals stiffness as a never before differing treatment modality. Drugs of this kind developed from 2 companies have been found to offer Neuroprotection, reduce inflammation and increase needed blood flow to the optic nerve. Combo surgeries involving micro values implanted as an adjunct to cataract surgery now exists , however this is of yet not a common frontline glaucoma treatment approach.
THE Modern F.A. or Digital Fluorescein Angiographer - When an eye undergoes Fluorescein Angiography what is being examined is the retinal and choroidal circulation utilizing a tracing Fluorescein Dye to evoke a digitized record called an Angiogram. Here once the Dye has been administered into a vein you are going to record the Fluorescence either Hyper or Hypo over 20 or so seconds. There will be specific stages of a Fluorescein Angiography with certain expected results at each stage. If something does Hyperfluoress when it should not at phase you have leakage or a detachment. If something does Hypofluoress instead of Hyperfluoress you have a blockage. The F.A. is valuable in Diabetic Retinopathy, Vein occlusions, disc edema, addressing retinal tumors ect. Very valuable but certainly invasive compared to HRT’s and OCT’s. The F.A. is the sole domain of a Retinal Specialist, which currently number 30 or so in B.C. where as the The High Def OCT is utilized by some O.M.Ds. and most O.Ds. as the tool of choice in the coordinated management of Glaucoma, and the detection and management of a vast array of retinal anomalies; especially ongoing or detecting events effecting one’s Macular Health.
